Scientists at Duke-NUS Medical School, in collaboration with an international consortium of partner institutions, have achieved a monumental breakthrough in neuroscience, assembling one of the most comprehensive single-cell maps ever created for the developing human brain. This pioneering atlas, dubbed BrainSTEM (Brain Single-cell Two tiEr Mapping), meticulously identifies nearly every cell type within the intricate neural landscape, meticulously records their unique genetic signatures, and illuminates the complex dynamics of how these cells grow, mature, and interact with one another. Crucially, the research also provides a rigorous comparative analysis of leading laboratory methodologies for producing high-quality neurons, a critical advancement poised to accelerate the development of innovative new therapies for debilitating neurological conditions such as Parkinson’s disease and a spectrum of other brain disorders.
The Global Burden of Neurodegenerative Diseases and the Promise of Cell Therapy
Neurodegenerative diseases represent a significant and growing global health challenge, characterized by the progressive loss of structure or function of neurons, leading to cognitive decline, motor dysfunction, and profound impacts on quality of life. Among these, Parkinson’s disease stands as a particularly prevalent and devastating condition. In Singapore, it is the second most common neurodegenerative disorder, affecting approximately three in every 1,000 individuals aged 50 and above. Globally, the incidence and prevalence of Parkinson’s disease are projected to rise dramatically due to aging populations, with estimates suggesting over 10 million people worldwide are currently living with the condition. The economic burden is equally staggering, encompassing direct medical costs, indirect costs from lost productivity, and the immense non-economic costs of reduced quality of life for patients and their caregivers.
At its core, Parkinson’s disease is characterized by the progressive degeneration of midbrain dopaminergic neurons, specialized nerve cells located in the substantia nigra region of the brain. These neurons are indispensable for producing and releasing dopamine, a neurotransmitter vital for regulating movement, motivation, and learning. The loss of these critical neurons leads to the hallmark motor symptoms of Parkinson’s, including tremors, bradykinesia (slowness of movement), rigidity, and postural instability, as well as a host of non-motor symptoms like cognitive impairment, sleep disturbances, and depression. Current treatments primarily focus on symptom management, with levodopa being the most effective medication to replenish dopamine levels. However, these therapies offer symptomatic relief rather than a cure, and their long-term use can lead to complications such as dyskinesias (involuntary movements) and "wearing-off" phenomena.
The immense promise of cell therapy in Parkinson’s disease lies in the potential to replace these lost dopaminergic neurons, fundamentally addressing the root cause of the condition. By implanting healthy, laboratory-grown neurons into the affected brain regions, researchers hope to restore dopamine production and communication, thereby alleviating symptoms and potentially halting disease progression. However, translating this promise into effective and safe clinical treatments has been fraught with challenges, primarily the difficulty in generating pure, functionally authentic dopaminergic neurons in sufficient quantities for transplantation, and the critical need to avoid the unintended production of other cell types that could lead to adverse effects.
BrainSTEM: A Precision Mapping Revolution
Addressing these formidable challenges, the Duke-NUS-led team embarked on developing a sophisticated approach to clarify precisely how dopaminergic neurons form and mature, both in natural development and in laboratory settings. This led to the creation of BrainSTEM, a novel two-step mapping methodology designed to provide unprecedented resolution into the cellular composition of the human brain.
The journey to construct this atlas involved an extensive collaborative effort, with key partners including the University of Sydney, leveraging their expertise in neuroscience and computational biology. The initial phase of BrainSTEM involved profiling an astounding nearly 680,000 individual cells meticulously isolated from the fetal human brain. This first tier of mapping provided a broad, foundational chart of the entire cellular landscape during critical developmental stages, offering insights into the diversity and distribution of various neuronal and glial cell types across different brain regions. This unprecedented scale of data collection represents a significant leap forward from previous brain mapping efforts, which often relied on more generalized tissue analysis.
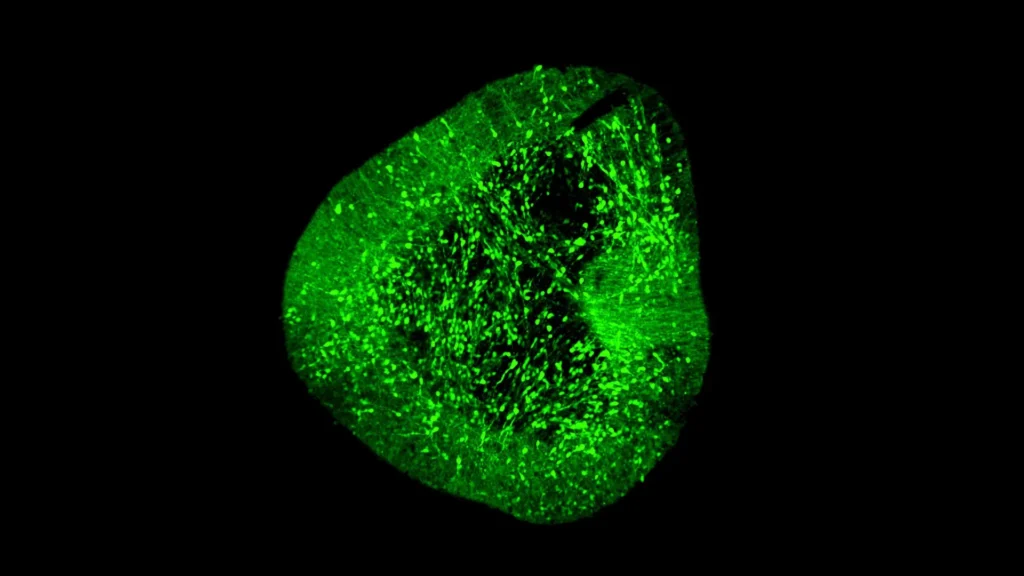
The second, higher-resolution tier of BrainSTEM then strategically targeted the midbrain, the specific region affected in Parkinson’s disease, with added precision. This focused approach allowed the researchers to pinpoint and characterize dopaminergic neurons with unparalleled detail, dissecting their unique genetic signatures and developmental trajectories. The resulting "comprehensive reference map" is more than just a static image; it is a dynamic blueprint that now serves as a global standard, providing an essential benchmark for evaluating how accurately laboratory models of midbrain development and neuron generation truly match the complex biology of the human brain. This meticulous validation is paramount for ensuring the safety and efficacy of future cell-based therapies.
Unmasking the Imperfections in Laboratory Models
A critical finding emerging from the BrainSTEM study, published in the esteemed journal Science Advances, sheds light on a significant hurdle in current neurodegenerative research. The study reports that several widely adopted methods used to grow midbrain cells in laboratory settings, while successful in generating some desired neuronal populations, also inadvertently produced unwanted cells originating from other brain regions. These "off-target" populations pose a substantial risk in the context of cell therapy, as their transplantation could lead to unforeseen side effects, including the formation of tumors or the integration of neurons with incorrect functions into the host brain, potentially exacerbating rather than alleviating symptoms.
These findings are a stark reminder of the complexity of neural development and underscore the necessity for rigorous quality control in cell manufacturing. The Duke-NUS team’s analysis clearly indicates that both existing experimental protocols for cell differentiation and the data analysis pipelines used to characterize these cells require significant refinement. The ability of BrainSTEM to precisely detect and quantify such off-target populations provides the critical tools needed to enhance the purity and safety of cell preparations, thereby paving a more reliable path towards clinical application.
Expert Perspectives on a Transformative Tool
The unveiling of BrainSTEM has generated considerable excitement within the scientific community, with the lead researchers highlighting its profound implications.
Dr. Hilary Toh, an MD-PhD candidate from the Neuroscience & Behavioural Disorders program at Duke-NUS Medical School and one of the first authors of the groundbreaking paper, articulated the direct clinical relevance of their work. "Our data-driven blueprint helps scientists produce high-yield midbrain dopaminergic neurons that faithfully reflect human biology," Dr. Toh explained. "Grafts of this quality are pivotal to increasing cell therapy efficacy and minimizing side effects, paving the way to offer alternative therapies to people living with Parkinson’s disease." Her statement underscores the immediate practical impact of BrainSTEM in refining the cell production process, making future therapies safer and more effective for patients desperately awaiting new treatment options.
Dr. John Ouyang, Principal Research Scientist from Duke-NUS’ Centre for Computational Biology and a senior author of the study, emphasized the unprecedented precision offered by BrainSTEM. "By mapping the brain at single-cell resolution, BrainSTEM gives us the precision to distinguish even subtle off-target cell populations," Dr. Ouyang noted. He further elaborated on the broader implications, stating, "This rich cellular detail provides a critical foundation for AI-driven models that will transform how we group patients and design targeted therapies for neurodegenerative diseases." This perspective highlights the synergistic potential of combining high-resolution biological data with advanced artificial intelligence, opening avenues for personalized medicine tailored to the unique molecular profiles of individual patients.
Assistant Professor Alfred Sun from Duke-NUS’ Neuroscience & Behavioural Disorders programme, also a senior author of the paper, reinforced the paradigm-shifting nature of BrainSTEM. "BrainSTEM marks a significant step forward in brain modelling. By delivering a rigorous, data-driven approach, it will speed the development of reliable cell therapies for Parkinson’s disease," Assistant Professor Sun asserted. He added, "We’re setting a new standard to ensure the next generation of Parkinson’s models truly reflects human biology." His comments emphasize the establishment of a new benchmark for accuracy and reproducibility in the field, crucial for accelerating translational research.
Professor Patrick Tan, Senior Vice-Dean for Research at Duke-NUS, offered an institutional perspective on the study’s profound impact. "This study redefines the benchmark — establishing multi-tier mapping as essential for capturing cellular detail in complex biological systems," Professor Tan stated. He concluded, "By revealing how the human midbrain develops in such detail, we will accelerate Parkinson’s research and cell therapy, delivering better care and offer hope to people living with the disease." Professor Tan’s remarks underscore the study’s foundational contribution to understanding complex biological systems, which in turn fuels the development of advanced therapeutic strategies.
Broader Impact and Future Horizons: From Open Science to Personalized Medicine
The researchers behind BrainSTEM are committed to fostering open science and accelerating global discovery. They plan to release their comprehensive brain atlases as openly accessible reference resources. Furthermore, the innovative multi-tier mapping approach itself will be provided as an "out-of-the-box" package, making this powerful methodology readily available to research laboratories worldwide. This commitment to open access is expected to democratize access to cutting-edge tools, enabling a wider scientific community to leverage BrainSTEM’s capabilities.
The versatility of BrainSTEM is one of its most compelling features. Because the underlying principles and techniques can be applied to isolate and characterize virtually any cell type within the brain, labs across the globe can utilize this framework to deepen insights into a multitude of neurological conditions, streamline their experimental workflows, and accelerate the pace of discovery across the entire spectrum of neuroscience research. This broad applicability extends beyond Parkinson’s disease, promising advancements in understanding conditions like Alzheimer’s disease, Huntington’s disease, stroke, and various developmental disorders.
Beyond direct cell therapy, the unprecedented detail provided by BrainSTEM holds immense potential for advancing drug discovery efforts. A precise understanding of the cellular composition, genetic signatures, and interaction networks within healthy and diseased brains can guide the identification of novel drug targets, enabling the development of more specific and effective small-molecule drugs or biologics. The integration of this rich cellular detail with AI-driven models, as highlighted by Dr. Ouyang, is poised to revolutionize how researchers approach disease modeling, patient stratification, and the design of truly personalized therapeutic interventions. This could lead to a future where treatments are tailored not just to a disease, but to an individual patient’s unique biological profile.
The development of BrainSTEM was made possible through significant collaborative funding, including support from programs such as the USyd-NUS Ignition Grant and the Duke-NUS Parkinson’s Research Fund, the latter made possible through a generous donation by The Ida C. Morris Falk Foundation. Such sustained investment in foundational research is crucial for driving the scientific breakthroughs that ultimately translate into tangible benefits for patients.
Duke-NUS Medical School continues to solidify its position as a global leader in medical research and education, driven by an unwavering commitment to improving patient care through scientific innovation. The BrainSTEM study is a testament to this mission, advancing ongoing efforts not only to understand the fundamental mechanisms governing brain function and development but also to pioneer and develop transformative new therapeutic strategies for a wide array of neurological conditions, offering renewed hope to millions worldwide.