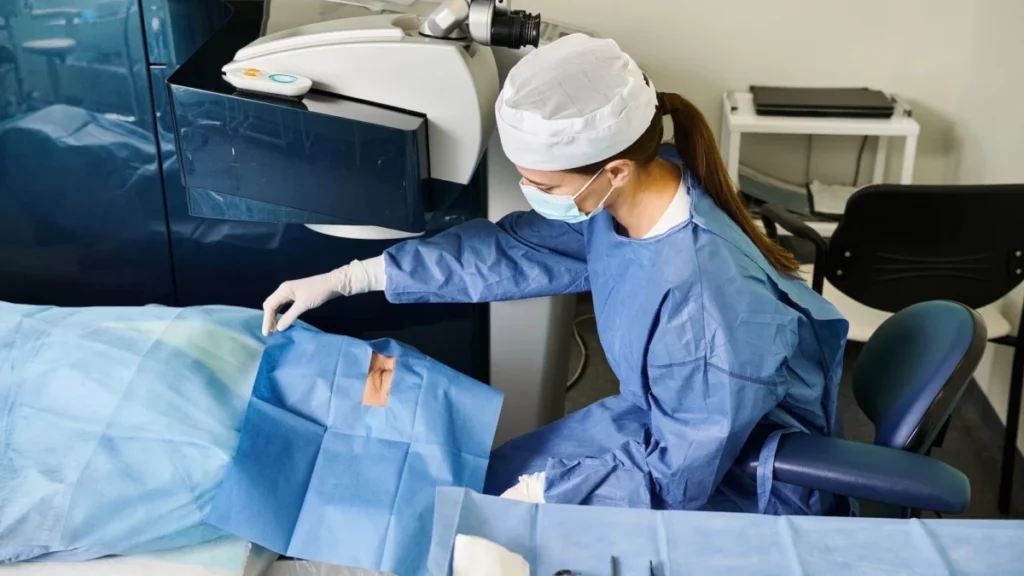
In a landmark development for the field of ophthalmology, Dr. Eric Rosenberg of SightMD has successfully performed the world’s first cataract surgery assisted by the Apple Vision Pro, signaling a potential shift in how complex medical procedures are executed and taught. While Apple’s flagship spatial computing headset has faced significant headwinds in the consumer market since its February 2024 launch, its integration into the operating room suggests a robust second life for the device as a high-precision medical tool. The procedure, which took place in October 2025, utilized a custom-built software platform known as ScopeXR, allowing Dr. Rosenberg to leverage the headset’s high-resolution displays and augmented reality capabilities to enhance surgical precision and facilitate real-person collaboration.
Cataract surgery is one of the most common medical procedures globally, with over 20 million operations performed annually. It requires extreme precision, as surgeons must remove the eye’s clouded natural lens and replace it with an artificial intraocular lens. Traditionally, this is done using high-powered surgical microscopes that require the surgeon to maintain a fixed, often uncomfortable physical posture for extended periods. By transitioning to a mixed-reality interface, Dr. Rosenberg has demonstrated that surgeons can maintain a more ergonomic position while accessing a wealth of digital data overlaid directly onto their field of view.
A New Paradigm for Surgical Visualization
The success of the procedure rests on the synergy between Apple’s hardware and the ScopeXR software. Dr. Rosenberg, a New England-based surgeon specializing in cornea, cataract, and refractive surgery, co-developed this "mixed reality surgical platform" to bridge the gap between traditional surgical imaging and modern spatial computing. The system functions by taking real-time data feeds from 3D digital microscopes and other diagnostic equipment within the operating room and streaming them directly into the Vision Pro headset.
The result is a stereoscopic 3D view of the surgical site that offers depth perception far superior to traditional 2D monitors. Furthermore, the augmented reality (AR) features of the Vision Pro allow the surgeon to overlay patient vitals, pre-operative scans, and real-time biometric data directly onto the workstation. This eliminates the need for the surgeon to look away from the patient to check secondary monitors, a move that minimizes distraction and reduces the risk of error during critical moments of the operation.
Dr. Rosenberg has reported that since the initial October 2025 procedure, he has used the device to assist in hundreds of additional cases. According to a press statement released by SightMD, the technology "democratizes access to expertise." By utilizing the Vision Pro’s advanced camera systems and internet connectivity, Dr. Rosenberg can broadcast his exact point of view to consultants, medical students, or fellow surgeons anywhere in the world. This "tele-mentoring" capability allows a specialist in New York to provide real-time guidance to a resident in a rural clinic, potentially saving the vision of patients who would otherwise lack access to top-tier surgical talent.
The Chronology of Spatial Computing in Medicine
The adoption of the Apple Vision Pro in the operating room did not happen in a vacuum. It is the result of a multi-year evolution in wearable technology and several key milestones in the medical field.
In February 2024, Apple released the Vision Pro to a domestic audience, marketing it as the dawn of "spatial computing." Despite the initial hype, the $3,499 price point and the lack of a "killer app" for casual users led to lackluster sales. By late 2024, reports emerged that many early adopters were returning the device, citing weight issues and a lack of practical utility. However, the medical community saw potential where the general public saw a novelty.
The first major breakthrough occurred in September 2024, when Dr. Santiago Horgan, a surgeon at UC San Diego Health, used the Vision Pro during a paraesophageal hernia repair. Dr. Horgan’s success proved that the headset’s 4K micro-OLED displays provided the clarity necessary for internal surgery. Following that milestone, the device was gradually integrated into other specialties, including treatments for acid reflux and obesity.
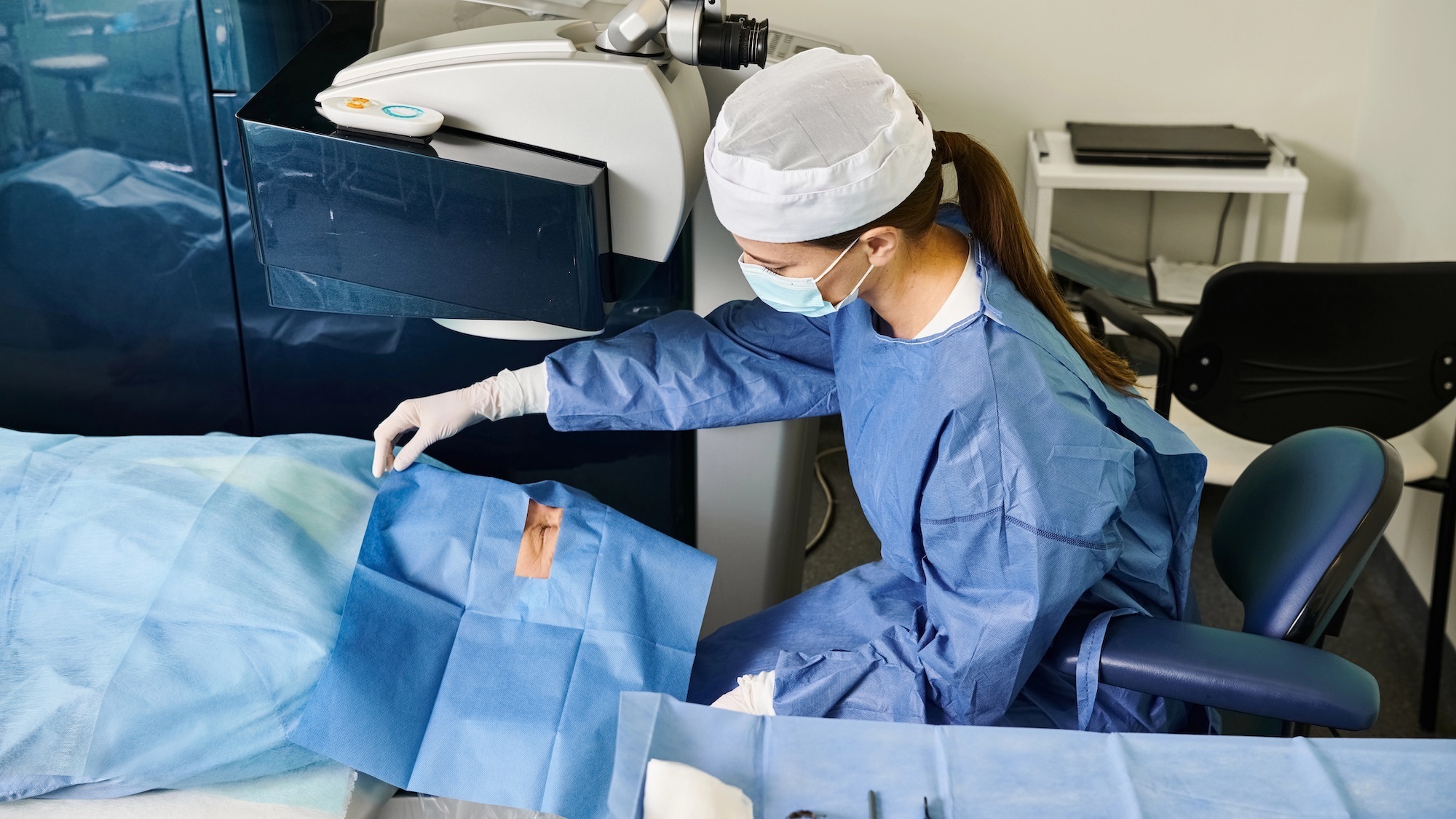
By the time Dr. Rosenberg applied the technology to ophthalmology in October 2025, the groundwork had been laid. Earlier attempts to use devices like Google Glass or Microsoft HoloLens in surgery had largely failed due to technical limitations. Google Glass suffered from low resolution and a narrow field of view, while the HoloLens, though more advanced, struggled with latency and image registration. The Vision Pro’s 12-millisecond latency and best-in-class resolution addressed these specific pain points, making it a viable candidate for the high-stakes environment of eye surgery.
Technical Superiority and the Economic Paradox
One of the most surprising aspects of the Vision Pro’s medical adoption is its cost-effectiveness. While $3,500 is prohibitively expensive for a consumer entertainment device, it is remarkably affordable within the context of medical infrastructure. Traditional high-end surgical displays and digital microscopy systems can cost hospitals anywhere from $50,000 to over $200,000.
The Vision Pro offers a comparable, and in some ways superior, visual experience at a fraction of that cost. This economic reality is particularly significant for regional and community hospitals operating on tight budgets. The ability to upgrade an operating room’s visualization capabilities for the price of a high-end laptop represents a significant shift in healthcare economics. Furthermore, the device’s portability allows it to be moved between operating rooms with ease, unlike bulky, stationary microscope systems.
From a technical perspective, the Vision Pro’s M2 and R1 chips allow for the simultaneous processing of multiple data streams with negligible lag. In surgery, where a millisecond of delay between a hand movement and its visual representation can be catastrophic, this processing power is essential. The headset’s ability to track eye movements and hand gestures also allows surgeons to interact with digital menus and patient records without breaking the sterile field—a perennial challenge in the operating environment.
Official Responses and Future Implications
The medical community’s reaction to Dr. Rosenberg’s achievement has been one of cautious optimism. Proponents argue that we are entering an era where the "operating room of the future" will be defined by software and wearable interfaces rather than hardware-heavy consoles. "We are now able to bring the world’s best surgeon into any operating room, at any hour, from anywhere on the planet," Dr. Rosenberg noted in a recent press release.
However, challenges remain. Regulatory bodies such as the FDA continue to evaluate the long-term safety and efficacy of using consumer-grade hardware for primary surgical visualization. There are also concerns regarding data privacy and the security of streaming live surgical feeds over the internet. Ensuring that these systems are HIPAA-compliant and protected against cyber-attacks is a priority for developers like those at ScopeXR.
Industry analysts suggest that Apple may be pivoting its strategy in response to these developments. While consumer sales have stalled, the professional and enterprise sectors—particularly healthcare and engineering—are showing sustained interest. There is speculation that future iterations of the headset may include a "Medical Edition" with specialized sensors or enhanced sterilization features suited for clinical environments.
Conclusion: Reimagining the Surgical Landscape
The successful application of the Apple Vision Pro in cataract surgery marks a turning point in the intersection of technology and healthcare. It transforms the headset from a maligned consumer product into a tool of profound social and clinical utility. By providing surgeons with enhanced 3D visualization, real-time data overlays, and global collaboration capabilities, the technology is poised to improve patient outcomes and accelerate medical training.
As Dr. Rosenberg and his colleagues at SightMD continue to refine the ScopeXR platform, the lessons learned in the operating room may eventually trickle back down to the consumer market, leading to lighter, more efficient devices. For now, however, the Vision Pro has found its most compelling use case not in the living room, but in the hands of those dedicated to saving and restoring human sight. The "reimagined operating room" is no longer a futuristic concept; it is a current reality, proving that even a commercial "flop" can change the world when placed in the right hands.











